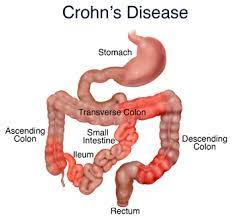
Crohn’s disease is a chronic inflammatory bowel disease (IBD) that causes inflammation in your digestive tract. This inflammation can occur anywhere along the digestive system, but most commonly affects the small intestine and large intestine (colon).
Unlike some illnesses with visible symptoms, Crohn’s can be an invisible illness. While some people experience outward signs of illness during flare-ups, others may not show outward symptoms.
Here’s a breakdown of Crohn’s disease:
Causes: The exact cause is unknown, but it’s likely a combination of factors like genetics, immune system response, and environmental triggers (smoking being a major one).
Symptoms: These can vary but commonly include:
- Diarrhea
- Abdominal pain and cramping
- Urgent need for bowel movements
- Rectal bleeding
- Weight loss
- Fatigue
- Anemia
- Mouth sores
How is Crohn’s disease diagnosed?
Diagnosing Crohn’s disease often involves a multi-step process because there’s no single definitive test. Doctors aim to rule out other conditions with similar symptoms and identify the characteristic signs of Crohn’s. Here’s a breakdown of the typical diagnostic approach:
-
Medical History and Physical Exam: Your doctor will discuss your symptoms in detail, including frequency, severity, and any other digestive issues. They will also perform a physical exam to check for abdominal tenderness or swelling.
-
Laboratory Tests: Blood tests can reveal signs of inflammation, anemia (common in Crohn’s), or nutritional deficiencies. Stool tests may be done to rule out infections or parasites.
-
Imaging Tests: X-rays, upper gastrointestinal (GI) series, CT scans, and MRIs can visualize the digestive tract and look for blockages, inflammation, or narrowing in the intestines. These tests might involve consuming a contrast material that helps the images show the intestines more clearly.
-
Intestinal Endoscopy: This is often the most conclusive diagnostic tool. Procedures like colonoscopy or capsule endoscopy allow doctors to directly examine the lining of the digestive tract for signs of inflammation, ulcers, or abnormal tissue. During a colonoscopy, a small tissue sample (biopsy) can be taken from suspicious areas for further analysis under a microscope. This biopsy can definitively confirm the presence of Crohn’s disease by identifying characteristic abnormalities.
Here are some additional points to consider:
- The specific tests used will depend on your individual situation and symptoms.
- Diagnosis may not always be immediate, especially if your symptoms are mild.
- If the initial tests are inconclusive, further investigation may be needed.
It’s important to consult with a gastroenterologist, a doctor specializing in digestive disorders, for proper diagnosis and management of Crohn’s disease.
Can Crohn’s disease be confused with other illnesses?
Yes, Crohn’s disease can be confused with other illnesses because several conditions share similar symptoms. Here’s why it can be tricky to diagnose:
-
Shared Symptoms: Diarrhea, abdominal pain, cramping, and urgency to have a bowel movement are common in Crohn’s, but also occur in other digestive disorders.
-
Location of Inflammation: Since Crohn’s can affect various parts of the digestive tract, the specific symptoms can vary, making it even more challenging to pinpoint the exact cause.
Here are some conditions that Crohn’s disease can be mistaken for:
-
Ulcerative Colitis: This is another IBD, but inflammation is limited to the inner lining of the colon. While symptoms can be similar, Crohn’s often involves deeper layers of the digestive tract and can skip patches (patchy inflammation) unlike ulcerative colitis which is typically continuous.
-
Irritable Bowel Syndrome (IBS): IBS causes abdominal pain, cramping, bloating, and diarrhea or constipation, but there’s no inflammation present. Unlike Crohn’s, IBS symptoms are often triggered by stress or certain foods.
-
Microscopic Colitis: This condition involves chronic inflammation limited to the inner lining of the colon, but only visible under a microscope.
-
Celiac Disease: This autoimmune reaction to gluten (a protein in wheat, barley, and rye) can cause diarrhea, weight loss, and fatigue, mimicking Crohn’s. However, celiac disease has a specific blood test and responds well to a gluten-free diet, unlike Crohn’s.
-
Infections: Bacterial, viral, or parasitic infections can cause symptoms similar to Crohn’s, but a stool test can usually differentiate them.
Why is an accurate diagnosis important?
While many conditions share similar symptoms, the treatments and long-term management strategies differ significantly. An accurate diagnosis ensures you receive the most appropriate treatment plan for your specific condition.
What tests are used to diagnose Crohn’s disease?
Diagnosing Crohn’s disease typically involves a multi-step approach using a combination of tests to rule out other conditions and identify the characteristic signs of Crohn’s. Here’s a breakdown of the most common tests used:
-
Medical History and Physical Exam: This is the first step. Your doctor will discuss your symptoms in detail, including frequency, severity, and any other digestive issues they may have noticed. They will also perform a physical exam to check for abdominal tenderness or swelling.
-
Laboratory Tests: These blood tests can reveal signs of inflammation in the body, anemia (common in Crohn’s disease), or nutritional deficiencies. Stool tests may also be done to rule out infections or parasites that could be causing similar symptoms.
-
Imaging Tests: X-rays, upper gastrointestinal (GI) series, CT scans, and MRIs can help visualize the digestive tract and look for blockages, inflammation, or narrowing in the intestines.
- X-rays: While not always definitive for Crohn’s, X-rays can reveal blockages or complications.
- Upper GI Series: This involves drinking a chalky liquid (barium) that coats the digestive tract, allowing doctors to see abnormalities on an X-ray.
- CT Scans: These detailed X-ray images can provide a clearer picture of the digestive tract and surrounding tissues.
- MRIs: Magnetic resonance imaging scans use radio waves and magnets to create detailed cross-sectional images of the body. They can be helpful in visualizing inflammation and complications, especially in the small intestine which can be difficult to assess with other tests.
-
Intestinal Endoscopy: These procedures allow doctors to directly examine the lining of the digestive tract for signs of inflammation, ulcers, or abnormal tissue.
- Colonoscopy: A flexible tube with a camera is inserted through the anus to examine the rectum and colon. During a colonoscopy, a small tissue sample (biopsy) can be taken from suspicious areas for further analysis under a microscope. This biopsy can be crucial for definitively diagnosing Crohn’s by identifying characteristic abnormalities.
- Capsule Endoscopy: In this procedure, you swallow a small capsule containing a camera that takes pictures as it travels through your digestive tract. This can be helpful for examining the small intestine, which is difficult to reach with a colonoscopy.
Remember, the specific tests used will depend on your individual situation and symptoms. Your doctor will choose the tests that are most likely to provide a clear diagnosis. It’s also important to note that diagnosis may not always be immediate, especially if your symptoms are mild. If initial tests are inconclusive, further investigation may be needed.
Treatment and Management:
Crohn’s disease is a chronic inflammatory bowel disease (IBD) with no cure, but there are treatments that can effectively manage symptoms and improve quality of life. Here’s an overview of the different treatment approaches:
1. Medications:
- Aminosalicylates (5-ASAs): These medications help reduce inflammation in the digestive tract. They are commonly used to treat mild to moderate Crohn’s disease and to maintain remission.
- Corticosteroids: These powerful drugs quickly reduce inflammation but are typically used short-term due to potential side effects like weight gain, bone loss, and high blood pressure.
- Immunomodulators: These medications suppress the immune system’s response and are often used to maintain remission and prevent flare-ups. They can take weeks or months to show their full effect.
- Antibiotics: These medications may be used to treat infections or fistulas (abnormal connections between the intestines and other organs) that can occur as complications of Crohn’s disease.
- Biological medications: These newer drugs target specific parts of the immune system involved in inflammation. They are typically used for moderate to severe Crohn’s disease or when other medications haven’t been effective.
2. Surgery:
Surgery may be necessary in some cases of Crohn’s disease, such as:
- To remove a damaged section of the intestine
- To treat complications like bowel obstructions or fistulas
- To improve quality of life if medical management is not effective
3. Diet and Nutrition:
There’s no one-size-fits-all diet for Crohn’s disease, but some dietary modifications can help manage symptoms and promote healing:
- Identifying food triggers: Some people find that certain foods worsen their symptoms. Keeping a food diary can help identify these trigger foods which can then be avoided or limited in the diet.
- Low-residue diet: During flare-ups, a low-residue diet that is easily digested may be recommended. This involves limiting high-fiber foods, dairy products, and fatty foods.
- Staying hydrated: Diarrhea can lead to dehydration, so it’s important to drink plenty of fluids throughout the day.
- Nutritional deficiencies: Crohn’s disease can make it difficult to absorb nutrients properly. Your doctor may recommend dietary supplements to ensure you’re getting the vitamins and minerals you need.
4. Stress Management:
Stress can worsen Crohn’s symptoms, so finding healthy ways to manage stress is important. Here are some strategies that may be helpful:
- Relaxation techniques like deep breathing, yoga, or meditation
- Exercise
- Getting enough sleep
- Talking to a therapist or counselor
5. Support Groups:
Connecting with others who understand the challenges of living with Crohn’s disease can be a great source of support and encouragement. There are many online and in-person support groups available.
Remember, treatment for Crohn’s disease is individualized. What works for one person may not work for another. It’s important to work closely with your doctor to develop a treatment plan that is right for you.
Living with Crohn’s
Living with Crohn’s disease can be challenging, but with the right approach, you can still maintain a good quality of life. Here are some key aspects to consider:
Managing Flare-ups:
- Early intervention: Recognizing the signs of a flare-up early and following your doctor’s instructions for managing it can minimize its impact on your daily life.
- Communication with your doctor: Keeping your doctor informed about your symptoms and any changes you experience is crucial for adjusting your treatment plan as needed.
Lifestyle Adjustments:
- Diet: As discussed earlier, identifying trigger foods and following a dietary plan that works for you can significantly reduce symptoms. A registered dietitian can help create a personalized plan.
- Stress management: Chronic stress can exacerbate Crohn’s symptoms. Finding healthy ways to manage stress, like relaxation techniques or exercise, is essential.
- Sleep: Getting enough quality sleep is important for overall health and can also help manage Crohn’s symptoms.
- Maintaining relationships: Open communication with family and friends about your condition can foster understanding and support. Support groups can also be a valuable resource for connecting with others who understand the challenges of Crohn’t disease.
Emotional Wellbeing:
- Coping with chronic illness: Living with a chronic condition like Crohn’s can be emotionally draining. Don’t hesitate to seek professional help from a therapist or counselor if you’re struggling to cope.
- Staying positive: Maintaining a positive outlook can significantly improve your quality of life. Focus on the things you can control and celebrate your victories, no matter how small.
Advocacy and Awareness:
- Educate yourself: Learning as much as you can about Crohn’s disease empowers you to manage your condition effectively.
- Raise awareness: Talking openly about Crohn’s disease can help raise awareness and understanding of this condition.
- Support research: Getting involved with advocacy groups or research initiatives can contribute to finding better treatments and ultimately a cure for Crohn’s disease.
Remember, you are not alone. Many people live fulfilling lives with Crohn’s disease. By following a comprehensive management plan, making healthy lifestyle choices, and staying positive, you can thrive despite this chronic condition.
Resources:
- The Crohn’s & Colitis Foundation: https://www.crohnscolitisfoundation.org/
- The National Institute of Diabetes and Digestive and Kidney Diseases: https://www.niddk.nih.gov/health-information/digestive-diseases/crohns-disease
Remember, if you suspect you may have Crohn’s disease, it’s crucial to see a doctor for diagnosis and treatment. Early intervention can significantly improve your quality of life.
thanks for reading…..!!!!

Your article helped me a lot, is there any more related content? Thanks!
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
Your article helped me a lot, is there any more related content? Thanks!